Care of the future, delivered today.
It is impossible to say when or who began cardiac anesthesiology, but it is possible to describe the evolution of this new medical specialty over the past seventy-five years. Cardiac Anesthesiology can be defined as the anesthetic practice focused on the preoperative, intraoperative and postoperative evaluation and management of patients with cardiac and intra- thoracic vascular disease.
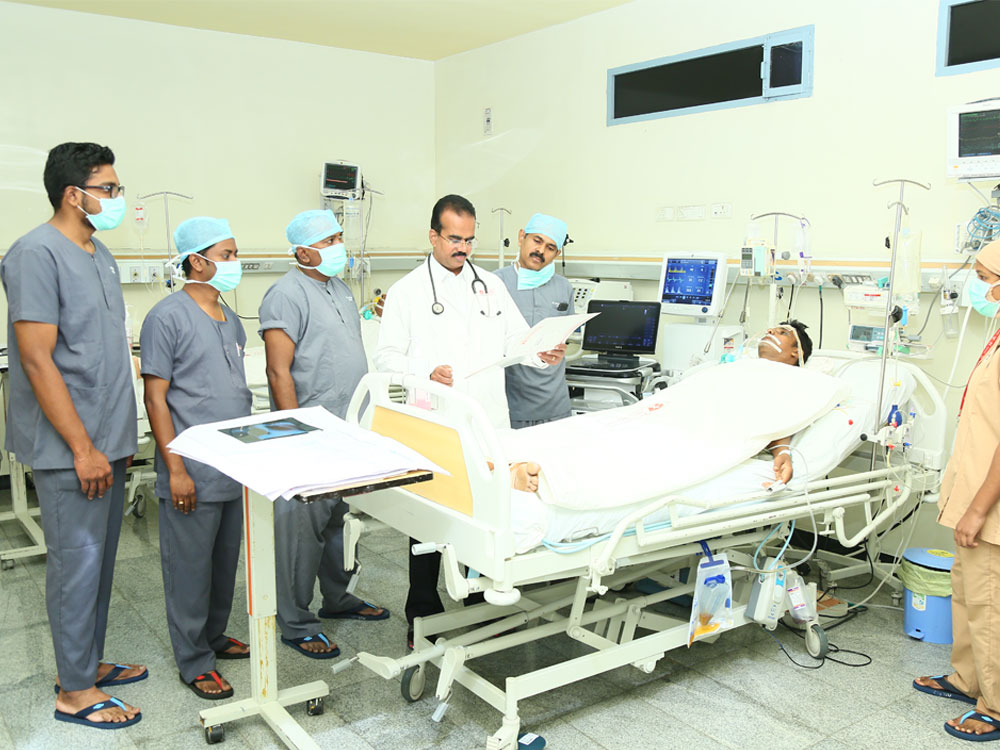
In our hospital, Cardiac Anesthesiology has evolved over the past 20 years. Our vision is to innovate and deliver high quality, cost effective anesthesia care and pain management; to create rewarding careers for our staff; and to develop leadership in the field of cardiothoracic anesthesia, Cardiac Critical care, Cardiovascular Diabetology and Cardiac rehabilitation.
STATISTICS:
The caseload comprises approximately 10, 000 cardiac procedures from 2012 to 2022. This covers the entire gamut of cardiothoracic anesthesia i.e. anesthesia for Coronary Artery Bypass surgery, Valvular heart surgery, congenital cardiac surgery and Thoracic & Vascular surgery.
About 85- 97% of our coronary revascularisation has been done on a beating heart, which requires quality care anesthesia and immense hemodynamic monitoring. In line with the advancements in cardiac surgery, our department performs valve repairs for suitable patients with good results. Cardiac anesthesiologists play a major role in performing peri-operative Transesophageal Echocardiography (TEE) thereby providing adequate assessment tailored to the pathology involved.
- A well-equipped theatre with an invasive multi-channel monitor including monitoring of ETCO2 and Cardiac Output.
- Nine-bedded CTS-ICU and Thirty bedded Cardiology ICU with multichannel monitors, latest Ventilators, and IABP machines.
- TransEsophageal Echocardiography.
- Thromboelastography (TEG)
- Extra Corporeal Membrane Oxygenation(ECMO)
- A dedicated, well-trained staff is always in attendance, and each patient receives individual care by a single nursing personnel.
- An anesthesiologist is available round-the-clock, and nothing is left to chance. This assures adequate post-operative care of the cardiac patient.
- In cardiac and post-cardiac surgical patients requiring prolonged mechanical ventilation, percutaneous tracheostomy is performed on a routine basis to facilitate secretion removal and to wean off from ventilator.

Dr. S. Kumar
MD, (Anaes)
Senior Consultant & Head

Dr. K. Balamurugan
MBBS, DA., DNB (Anaes)
Senior Consultant

Dr. Dhinakaran Daniel
MD, (Anaes)
Consultant

DR. BR. Bageerathi
MD.,(Anes)
Registrar